About the author
Ruth Barratt is an Infection Prevention and Control Consultant and Health Quality Advisor RN, BSc, MAdvPrac (Hons), CICP-E. Ruth provides advice and training to Reynard Health Supplies concerning the needs of infection prevention and control professionals and developments in the industry.
Ruth originally trained as a registered nurse in the UK but preventing infections has been her specialised field of work in NZ and Australia for over 20 years. She obtained her Masters in Infection Control and Prevention through Griffith University and is currently undertaking a PhD at the University of Sydney – again in the area of infection prevention
COVID-19: Tips on using personal protective equipment
for healthcare workers
The rapidly-spreading global pandemic of COVID-19 disease, caused by the novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is a key issue for infection prevention and control.
 Among the many outbreak control strategies introduced, the use of personal protective equipment (PPE) for healthcare workers caring for suspected or confirmed COVID-19 cases, is a key administrative infection prevention and control measure for staff and patient safety.
Among the many outbreak control strategies introduced, the use of personal protective equipment (PPE) for healthcare workers caring for suspected or confirmed COVID-19 cases, is a key administrative infection prevention and control measure for staff and patient safety.
Although PPE is commonly used, it is important that healthcare workers know how to use this equipment optimally and safely. In Australia and New Zealand, there are national and state guidelines for PPE use and many resources available online. PPE for COVID-19 is not new and many healthcare workers are familiar with the individual items. However general anxiety around COVID-19 has meant many staff require refresher training to feel competent in using the PPE safely.
Top tips for safe and optimal PPE use
1. Understand the transmission routes of the virus
COVID-19 is primarily spread through direct contact with droplets from an infected person’s cough or sneeze, or indirect contact by touching objects or surfaces that have been contaminated with cough or sneeze droplets from an infected person and then touching the face, especially mouth, nose or eyes. Therefor the primary routes of transmission are Droplet and Contact.
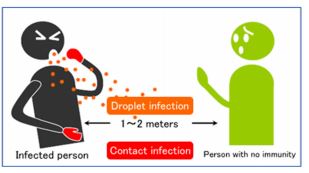
Airborne transmission of COVID-19 is not common unless an aerosol generating procedure is undertaken e.g. intubation, high-flow oxygen.
Note: taking respiratory swabs is NOT considered an aerosol-generating procedure.
2. Know what PPE is required
For droplet and contact precautions use the following PPE: 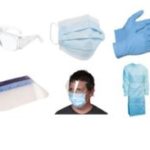
• Disposable impervious or semi-impervious gown
• Disposable gloves
• Protective eye wear
• Surgical mask
If an aerosol-generating procedure is performed, then use a N95/P2 mask and ensure it is fit-checked prior to entering the patient area.
3. Know how to put on (don) and take off (doff) your PPE correctly
Staff must be trained and competent in the skills for donning and doffing PPE correctly. It can be helpful to train with practical demonstration and allow users to practice themselves. Incorporating visual aids such as posters, videos or virtual reality can also be beneficial. Healthcare workers should continue to follow their organisation’s order for donning and doffing as the order can vary slightly from facility to facility.
Below are a some points to remember:
• Always tie gown at back – not at front.
• Pull gloves up over gown cuff.
• Position mask correctly on face – always fit check the seal of a P2 mask if using one.
• Incorporate hand hygiene into doffing process – always after gloves are removed and
always before removing facial protection.
• Avoid touching contaminated parts of the PPE during use and while doffing e.g. front of
gown, outside of gloves, front of mask and eye/face protection.
• Always discard disposable PPE after use – do not put mask in pocket, let it hang around
neck, or share with others.
• Clean re-usable goggles or eyewear after use.
• Remove mask last to protect the face.
Below is a Poster example showing the correct removal of PPE with surgical mask
(courtesy SCHN, Australia)